There are few things that test endurance, faith, the frontiers of medical knowledge in the context of limited resources, and stress management more intensely than working in a public hospital maternity ward. There is also no better place to learn and practise what quality healthcare can and should look like.

I would know. A few years ago, I was a medical officer working night shifts at Pumwani Hospital, a busy obstetric and referral hospital in Nairobi, and also one of the oldest maternity facilities in Kenya.
The labour ward in Pumwani was always at capacity, housing 70 or so pregnant women at any given time in various stages of active labour. The work of the floor medical officer, alongside the team of duty midwives, was to shepherd every single one of these women safely through the harrowing birth process to what would ideally be the successful delivery of a healthy, crying baby (or babies), finish with the afterbirth, and hand her back over to the regular ward for postpartum care.
Delivering a baby is very much like flying a plane: for the most part, everything happens as it should with minimal interference. But when it goes wrong, the situation can escalate from zero to one million in a matter of seconds. Unlike other healthcare personnel who mostly deal with one person at a time, staff in labour wards have to think about the entangled outcomes of both mother and baby simultaneously, and carry them both, as far as possible, and as quickly as possible, through unpredictable crises to stability.
Pumwani Maternity Hospital is located in Nairobi’s Eastlands area, and getting to work by public transport – heads bumping on matatu roofs as they dodged everything from open sewer holes to hawk-eyed policemen – felt worlds away from the flashier private facilities just a few kilometres away in the city’s leafier suburbs. Alongside maternity wards in more developed countries, these facilities all have one thing in common: a philosophy that values restoring physical health over care.
Healthcare with humanity
Merriam-Webster dictionary defines healthcare as “efforts made to maintain or restore physical, mental, or emotional wellbeing, especially by trained and licensed professionals”.
While it is clear that health services are geared towards ensuring decent physical outcomes, such as an end to pain, the idea of restoring mental and emotional wellbeing is very much in the wind for many. What is so often missing in both state-of-the-art hospitals in large urban centres, as in tiny rural clinics, has been the considered, tender focus that makes people feel deeply heard at all levels. With things as they are now, fair outcomes can be achieved with bare-bones technical competency and entry-level politeness.
Access to health services is a human right as defined by the World Health Organization, but our understanding of care needs to extend even beyond the singular provider’s ability to be compassionate. A regard for humanity is crucial as it forms the baseline, whether spoken or unspoken, for health service provision in any country. If our understanding is that human lives are measured in terms of productivity, then the body is no different from a car we have to be able to extract value from, and health service providers are mechanics, whose work it is to deliver functioning cars back onto the road.

The example of a car is deliberate: a car has no feelings that one has to care about. A human being, however, will feel shame when their bedpan has to be changed, is embarrassed to wear an ill-fitting medical gown which leaves their entire backs cold and naked, and is apprehensive about reporting illness to the workplace and potential loss of income. If the health services provider is to have a shot at restoring health, these are all issues that will have to be dealt with, alongside the symptoms that brought the individual over the clinic threshold.
A lack of engagement with these wider, very human concerns plays a significant role in what has been called the compassion crisis. There is plenty of literature to support the assertion that poor doctor-patient communication leads to increased spend on tests and images, sub-optimal patient self management, and non- or sub-adherence to drug protocols, all increasing the resource burden on health systems.
The 2020s have begun with the global shock that is the coronavirus pandemic, bringing to the fore the necessity of consistent, deliberate investment in the health sector – bearing in mind that all other sickness did not pause when Covid-19 arrived. It has become evident that even without the pandemic, health sectors across the globe were facing multiple crises. It is incumbent on us to get off this slippery slope, if we intend to move into the future with global health that is capable of handling needs in humanity that we have not even foreseen.
Some argue that healthcare gaps are a problem the market can fix, and so it is important to compare the roles of private and public healthcare systems.
The same public services rich nations see as a source of pride become foreign direct investment opportunities in developing nations, cannibalising failing public sectors. In countries such as Kenya, these private institutions have also served to position themselves as medical tourism hubs, offering quality care that prioritises everyone but the citizens. Meanwhile, senior African civil servants, whose salaries are paid by taxpayers, are notorious for seeking healthcare outside their borders simply because they can afford to. The public, in their stead, have to contend with crowded, under-resourced, deteriorating state facilities which they cannot opt out of. As such, because our leaders are not directly affected by the pressures of these fragile, bursting systems, they feel no pressure to reform them.
Because the bar is so low for public healthcare, the market does not have to do much better – or be held to a very high standard – to still be allowed to run. The mass privatisation of health services has therefore opened the door to the abuse of the public by the market, who will do the absolute least to make the absolute most in terms of profit. A profit motive of business is not wrong in and of itself, but we must be candid about the dysfunctions it leads to. Dignity is often sacrificed during these conflicts between private and public care in favour of the bottom line. As always, when dignity is for sale, the poorest and most marginalised people will suffer the most because they can’t afford to buy it.
When we say then that the practice of compassionate care must return to health service provision, we mean that it should be a baseline among the free offerings to each person, and not an in-app purchase. Even from a purely economic perspective, the data shows us that patients who are convinced that they are cared for, and provided with individualised and interactive care, get better faster, manage chronic conditions better, and are happier, more engaged workers.
When dignity is for sale, the poorest and most marginalised people will suffer the most
The value of an individual citizen is of course paramount, absolute, and immeasurable. Where we choose to see citizens only as economic value – contributors to gross domestic product – then minors, people living with disability, refugees, those living in poverty, or living with mental illness, and others whose bodies and minds are not immediately in full service to the wider state project, are considered expenses. Applying a value system around people as defined by the needs of the market alone will always be dangerous and dehumanising.
When driven by profit alone, care in health service provision will always remain a secondary consideration, if it is even put on the table. But there are other reasons why care is lacking even in wealthy countries, where larger numbers of people can afford to cover the costs of their health services and where the state supports those who can’t. One of these is gender roles and practice: in a gendered society, care is profoundly invisible and undervalued.
From the home to the workplace, caregiving is seen to be “women’s work”, with anyone in a caregiving role routinely underpaid and overworked. As a result, burnout among people doing care work is common. Health providers are much more prone than most to mental health challenges, and destructive coping mechanisms, causing inability to function both at work and as a person.
When we compare this with rampant understaffing in the sector, it means that relatively few people are tasked with an almost superhuman care burden. Medical schools cannot churn out enough doctors to meet current need, and those who do graduate are sucked up by cities, leaving rural populations vulnerable. We have normalised the extreme: across the vast majority of societies, health services providers are expected to give the most while being provided with the least – in much the same way as what’s demanded of women in the home.
How do we put the ‘care’ back in healthcare?
So where might we go from this increasingly untenable situation? How might we put “care” back into healthcare in this decade? There are three places where we could begin.
The first is a long overdue analysis and understanding of the condition of the health service provider. From Nairobi to Tokyo, Brisbane to Quito we must learn how to put care into the very systems and people we expect it from. Improving staff numbers, creating change in the work environment, recognising and managing the unavoidable stress, and fatigue so as to mitigate burnout. This matters for everyone, from the health services support, such as administrators, accountants and cleaners, all the way to the technicians, nurses, doctors and specialists.
Beyond addressing the individual workers, it is also high time health service provision moved away from the current doctor-headed hierarchies, which themselves are a relic of the time when most doctors were male and most nurses were female. Fostering interdisciplinary teams instead would diffuse the inordinate pressure on doctors to make solitary decisions, using opaque processes, and be responsible for these on their own. It would relieve the expectation on nurses to provide every ounce of emotional labour needed to help patients cope, and also elevate the expert knowledge of others who tend to remain unseen, such as pharmacists and technicians.

Secondly, healthcare education and practice needs to catch up to wider societal discourse around gender, race and class. Every day we gather more stories and evidence that should force us to face the ugly truth as illustrated in George Orwell’s well-known classic, Animal Farm: “All animals are equal, but some animals are more equal than others.” Due to implicit biases certain groups find their pain dismissed and their symptoms ignored. Depending on where in the world you are, you stand a chance of facing discrimination from health services because you are black or brown, a woman, queer or trans, young or old, belong to the wrong religious group, living in poverty or without the “right” documentation. Harmful stereotypes have clearly led to neglect, harm and general poor health outcomes. Just look at the trends in mortality from Covid-19 around the world, and you’ll see who’s most disenfranchised.
There must be interventions all the way from tertiary school level, to avail students of health sciences with essential coaching, as well as ongoing learning for qualified practitioners, that enables them to see the patient as a collaborating partner in their own healthcare, as opposed to in a “low-status/high-status” interaction in favour of the health provider.
Finally, we must engage more strongly with quaternary healthcare. Quaternary care, and notably quaternary prevention, which was devised in 1986 by a Belgian doctor, Marc Jamoulle, refers to “an action taken to identify a patient at risk of over-medicalisation, to protect him from new medical invasion, and to suggest to him interventions which are ethically acceptable”.
For a long time patients have been told that they must give birth or die in hospitals, which is often uncomfortable, necessitating endless and sometimes unnecessary monitoring by strangers, and sacrificing flexible and individualised attention in favour of regimented protocols that suit the health services more than they do the patient. Too often, also, medics understand the body as a binary of wellness and disease, when there is in fact a wide, grey spectrum in between.
A patient’s life and symptoms are always informed by where they live, what they believe and why, and what their support systems and close relationships look like. A quaternary care approach is deliberate about considering these, as well as only coming in with direct medical interventions when they are absolutely necessary.
People have been born, lived and aged, able-bodied or with disability, and died, without having to involve medical practitioners. Quaternary care remembers this way of living, and works to give some of this important control over their own lives back to the people. Care is possible beyond the shiny, white tiles and chlorine bleach fumes of a hospital.
During my many night shifts on the labour ward all those years ago, running from bed to bed in gumboots and scrubs, I often thought of the myriad traditional birth attendants all over Kenya and the African continent, who heal with potent herbs and gentle hands. I thought about the rising numbers of doulas around the world who kindly guide women in their own homes, via sms or over the internet, through abortions, miscarriages, deliveries and postpartum depression. These people do not have the power of large institutions funded by venture capitalists, full to the brim with shiny, smart gadgets – and for the most part, they don’t need it. What they do have, which is in critically low supply elsewhere, is compassion, understanding and care in abundance.
I’ve since transitioned out of clinical practice and into education and policy, and then into culture and the arts to understand the power of story better. While this new frontier of work makes me feel like I have been catapulted forward, medical practice is in many ways retreating back into itself: away from the public and towards technology; away from the complexities of holistic care and the possibilities therein and towards politics and bottom lines.
Besides the often prohibitive costs of accessing healthcare as we currently know it, people are also turning away in search of spaces where they can feel safer, more hopeful and dignified. This could be anywhere from ancestral herbal medicine practitioners, priests and spiritualists, to more secular micronutrient regimens and green juice “detox” diets as taught by viral YouTube videos. If health services, such as they are, intend to be part of a sustainable human future, it is time for them to make the main thing the main thing and turn back towards the people.
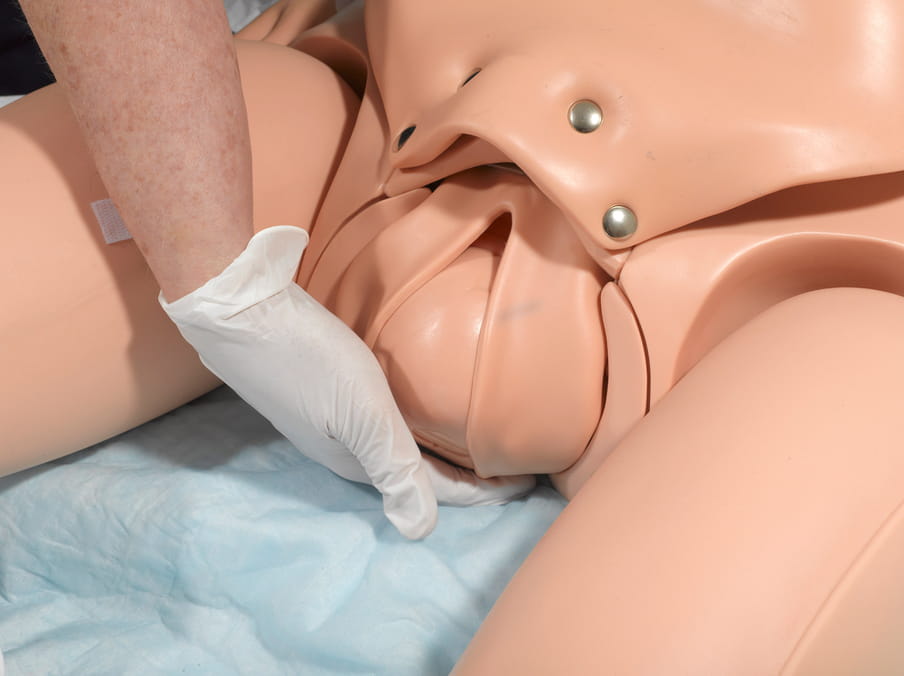
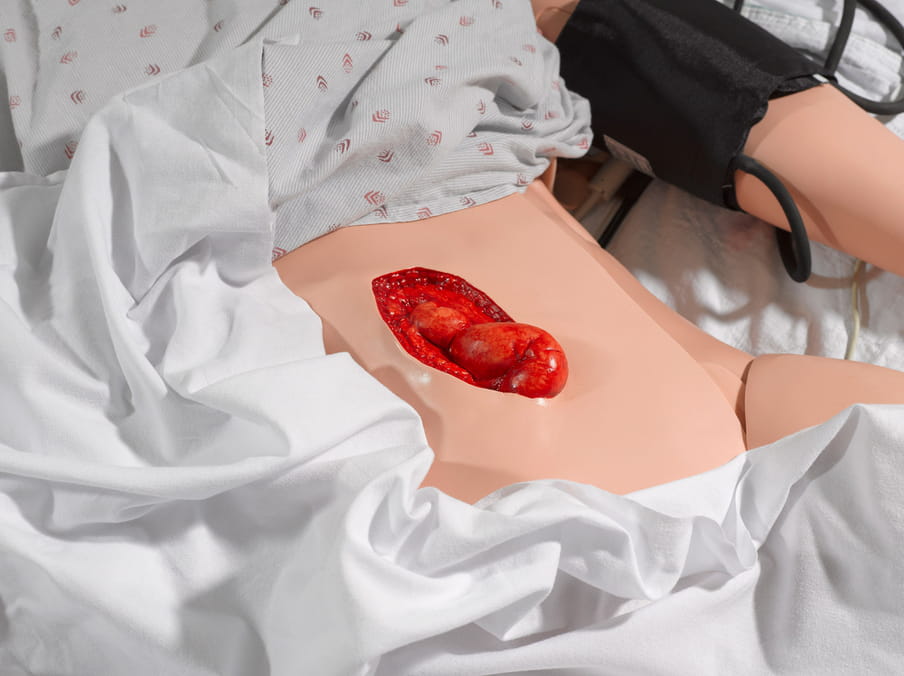
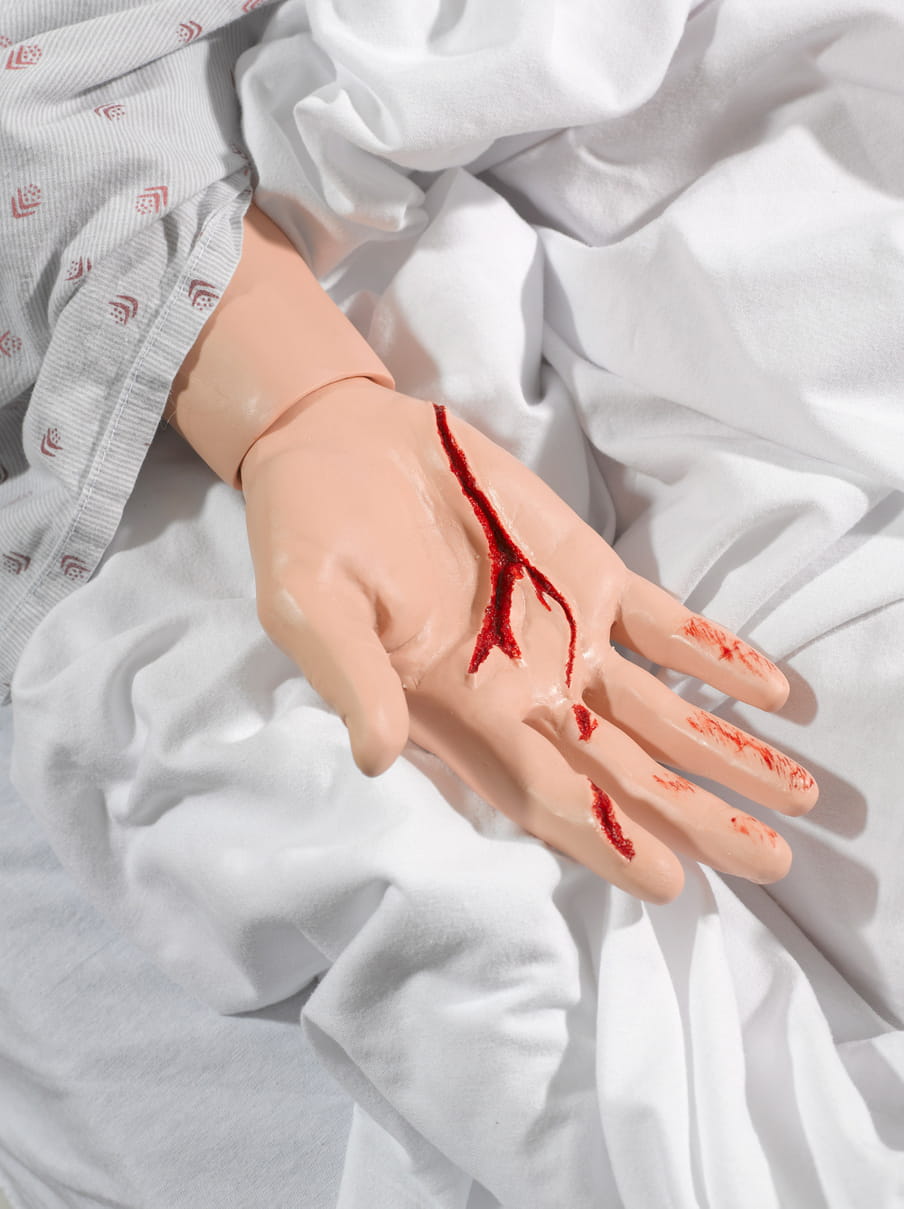
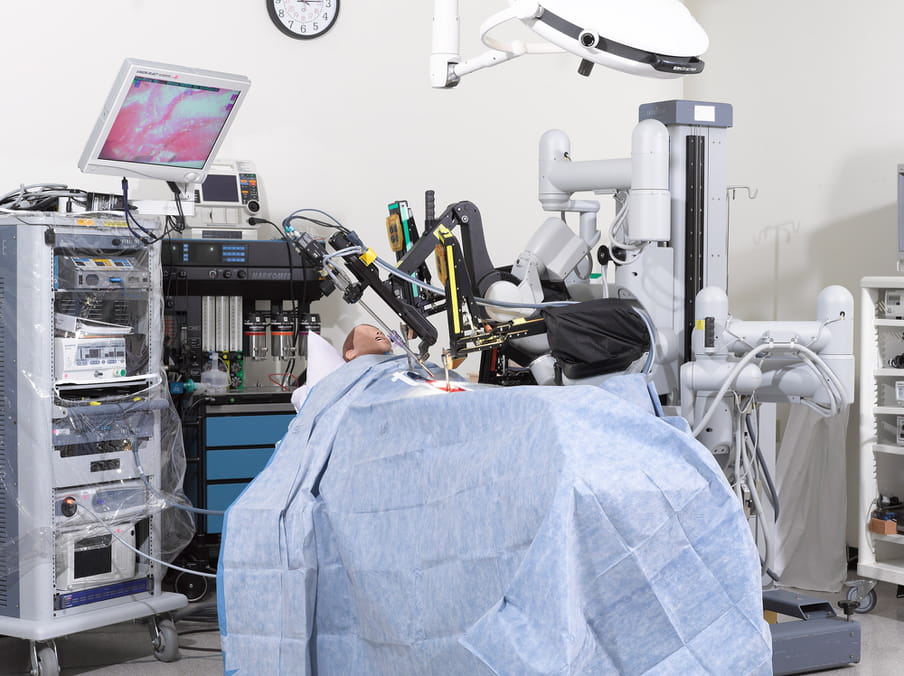
 About the images
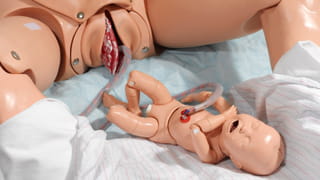
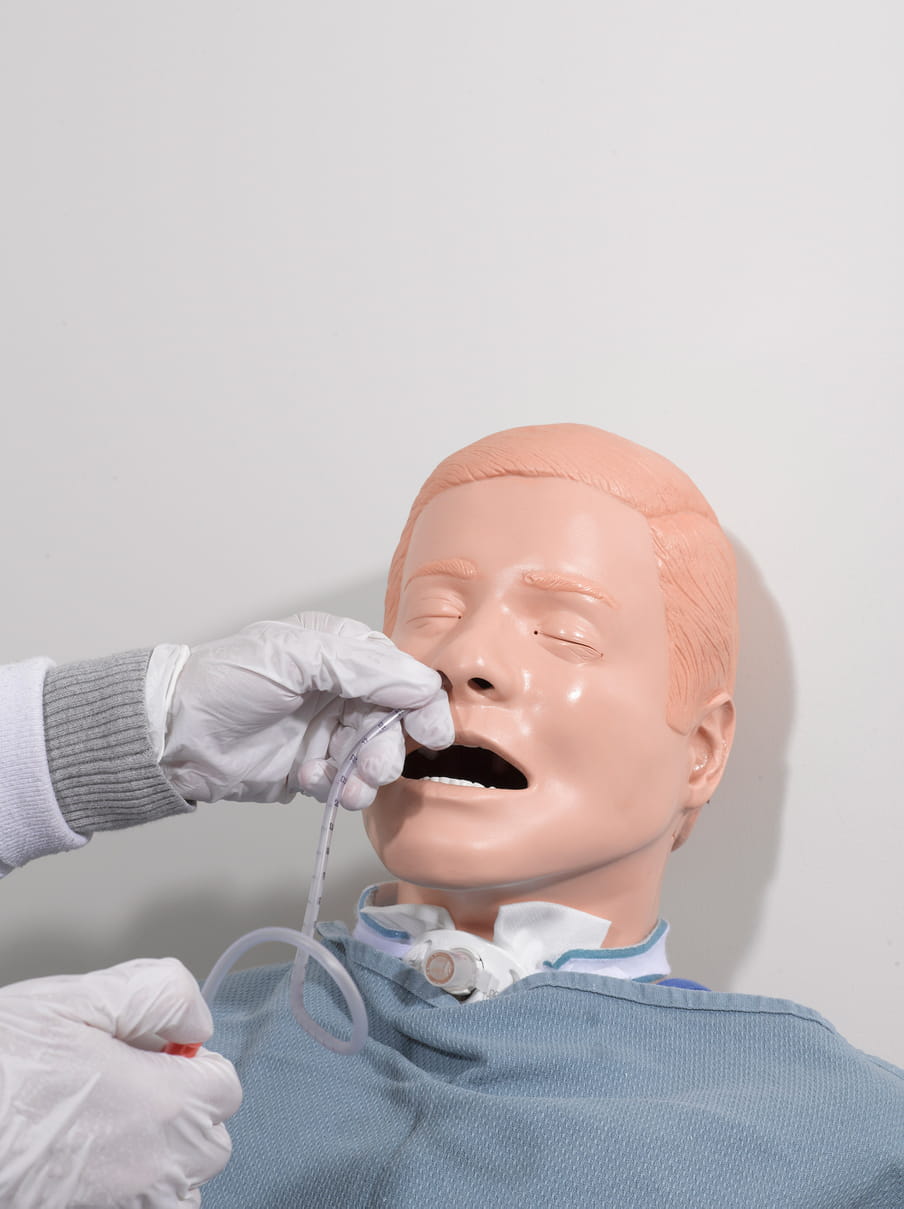
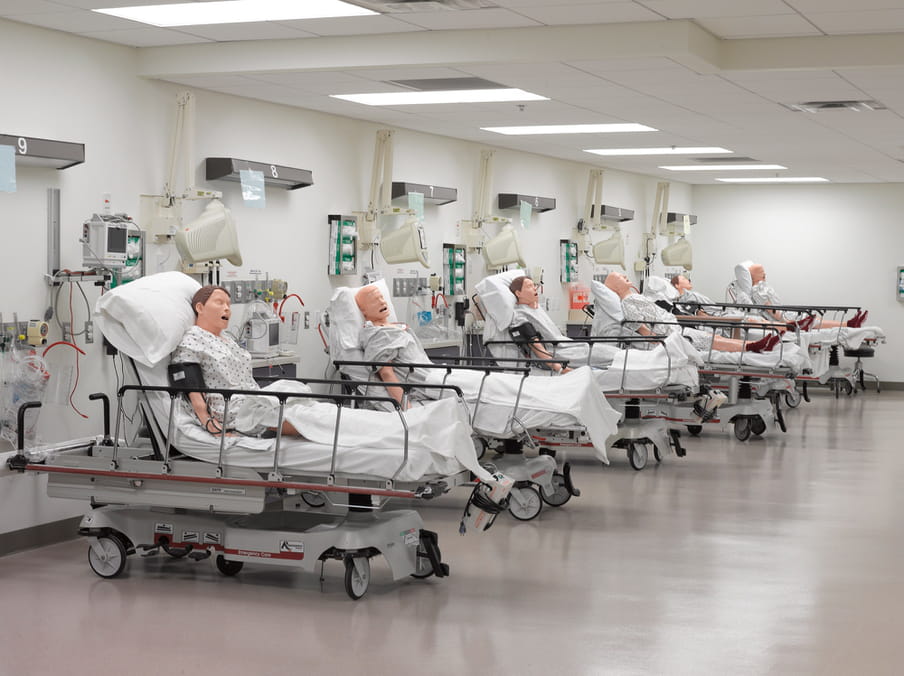
A hospital full of patients who give birth, bleed, moan or have surgery. But none of the patients have a heartbeat. Shot in a medical training facility for future doctors and nurses, Stier’s photos have an absurd quality. While the dummies might be crucial to teaching skills to future healthcare workers, they also symbolise what is left if every human element is taken out of healthcare: a bizarre spectacle that’s a tad scary. (Lise Straatsma, image editor)
About the images
A hospital full of patients who give birth, bleed, moan or have surgery. But none of the patients have a heartbeat. Shot in a medical training facility for future doctors and nurses, Stier’s photos have an absurd quality. While the dummies might be crucial to teaching skills to future healthcare workers, they also symbolise what is left if every human element is taken out of healthcare: a bizarre spectacle that’s a tad scary. (Lise Straatsma, image editor)
Dig deeper
 The time has come to take the self out of self-care
While the reminder to care for oneself can lead to improved wellbeing, the idea is increasingly commodified and weaponised against those who are most vulnerable. Here are four problems with our golden age of self-care.
The time has come to take the self out of self-care
While the reminder to care for oneself can lead to improved wellbeing, the idea is increasingly commodified and weaponised against those who are most vulnerable. Here are four problems with our golden age of self-care.
 The real reason we’re ad free (and six other questions from our members, answered)
What do we mean by constructive journalism? Why do we have members and not subscribers? And you get it, we’re ad free. But so what? Managing editor Eliza Anyangwe and founding editor Rob Wijnberg answer the seven most frequent questions we get about The Correspondent.
The real reason we’re ad free (and six other questions from our members, answered)
What do we mean by constructive journalism? Why do we have members and not subscribers? And you get it, we’re ad free. But so what? Managing editor Eliza Anyangwe and founding editor Rob Wijnberg answer the seven most frequent questions we get about The Correspondent.